#26 of
 EP Edge Journal Watch
EP Edge Journal Watch
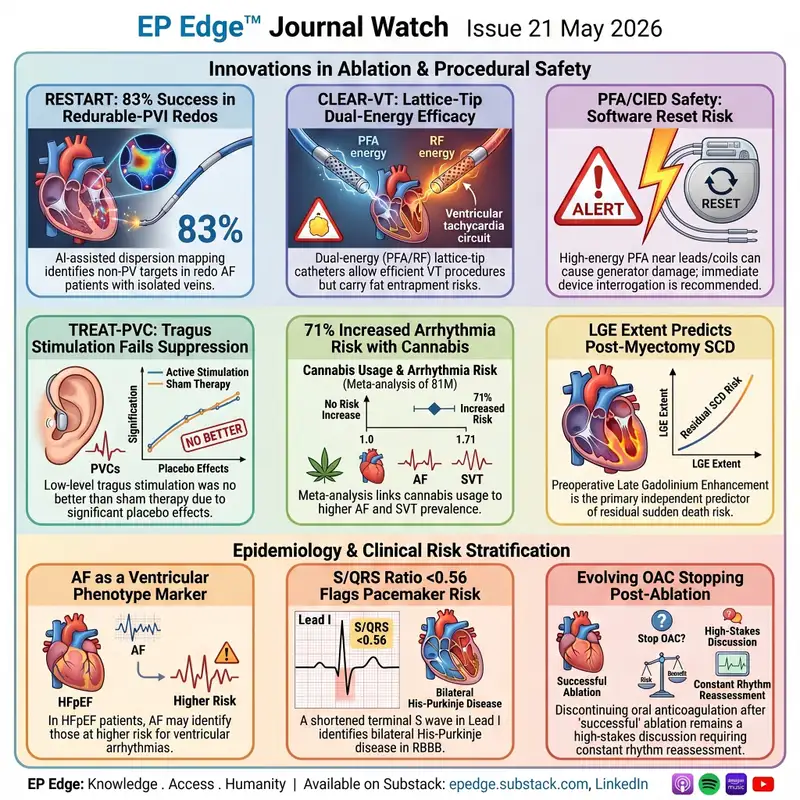
In this May 2026 episode of EP Edge™ Journal Watch, we review nine high-impact electrophysiology studies shaping contemporary EP practice. This issue covers AI-guided redo AF ablation, dual-energy lattice-tip ventricular arrhythmia ablation, pulsed field ablation safety in patients with cardiac implantable electronic devices, neuromodulation for PVC suppression, cannabis-associated atrial arrhythmia risk, sudden death risk after HCM myectomy, atrial fibrillation as a ventricular arrhythmia risk marker in HFpEF, post-ablation anticoagulation strategies, and a practical ECG marker for pacemaker risk in right bundle branch block.1. RESTART Trial: AI-guided redo AF ablation in patients with isolated pulmonary veins The RESTART trial examines one of the most difficult redo AF scenarios: recurrent symptomatic atrial fibrillation despite durable pulmonary vein isolation. The study evaluates whether AI-guided electrogram dispersion mapping can identify non-PV substrate and guide a more disciplined redo ablation strategy rather than relying on empirical lesion sets.2. CLEAR-VT: Dual-energy lattice-tip ablation for ventricular arrhythmias CLEAR-VT reports early U.S. experience using a dual-energy lattice-tip catheter capable of radiofrequency and pulsed field ablation for complex ventricular arrhythmias. The study is important because it highlights both the promise of broader lesion delivery in scar-related VT and the need for a new safety framework around device interaction, ventricular dosing, and substrate-specific limitations.3. PFA/CIED safety cluster: Device reset, generator damage, VF, and lead-mediated risk This section reviews a group of reports describing clinically relevant interactions between high-energy ablation systems and pacemakers, ICDs, CRT devices, leadless pacemakers, and ICD coils. The key issue is that PFA is tissue selective, but it is still an electrical therapy delivered in patients with conductive hardware, making pre- and post-procedure device interrogation, imaging awareness, and lesion planning essential.4. TREAT-PVC: Transcutaneous vagus nerve stimulation for PVC suppression TREAT-PVC tests whether low-level tragus stimulation can reduce symptomatic idiopathic PVC burden compared with sham stimulation. The central lesson is not simply whether neuromodulation works, but how strongly placebo effects, PVC variability, and potentially active sham physiology can affect device-based autonomic trials.5. Cannabis use and atrial arrhythmias: Systematic review and meta-analysis This large meta-analysis evaluates the association between recreational cannabis use and atrial arrhythmias, including atrial fibrillation, atrial flutter, atrial tachycardia, and SVT. The findings do not prove causality, but they make cannabis clinically relevant in arrhythmia history-taking, especially in younger patients, unexplained palpitations, AF, flutter, or SVT.6. Postmyectomy hypertrophic cardiomyopathy: Residual sudden death risk This CMR-based cohort evaluates predictors of sudden cardiac death after surgical septal myectomy in obstructive HCM. The key clinical message is that myectomy can relieve obstruction, but it does not erase myocardial fibrosis, so late gadolinium enhancement remains important in ICD and surveillance discussions.7. AF in HFpEF: Marker of ventricular tachyarrhythmia or cardiac arrest risk This study explores whether atrial fibrillation in HFpEF identifies patients at higher risk for ventricular tachyarrhythmias or cardiac arrest. It should not be interpreted as an ICD-indication study, but it raises an important hypothesis: AF in HFpEF may be a marker of deeper atrial-ventricular remodeling, fibrosis, autonomic dysfunction, or comorbidity clustering.8. Long-term antithrombotic strategies after AF ablation: Network meta-analysis of randomized trials This analysis addresses one of the most practice-sensitive questions in AF management: whether anticoagulation can be safely stopped after apparently successful AF ablation. The signal is provocative, but the boundary remains narrow because event rates are low and high-risk patients remain underrepresented; this is a shared-decision paper, not a broad permission slip to stop OAC.9. S/QRS ratio in lead I: ECG clue to pacemaker risk in RBBB This study examines whether the S-wave duration in lead I, expressed as a fraction of total QRS duration, can help identify patients with RBBB who may be at higher risk of requiring a pacemaker. The practical takeaway is simple: in RBBB, do not only measure QRS width—look carefully at lead I, because a short terminal S wave may suggest more diffuse His-Purkinje disease.Across all nine studies, the theme is consistent: modern electrophysiology is becoming more powerful, more data-driven, and more device-dependent, but the clinical edge still comes from judgment. EP Edge™ Journal Watch translates these studies into practical EP interpretation for electrophysiologists, cardiologists, EP fellows, APPs, and clinically engaged trainees.The full written issue, graphics, references, and subscription links are available through EP Edge™ Journal Watch on LinkedIn and Substack at epedge.substack.com.